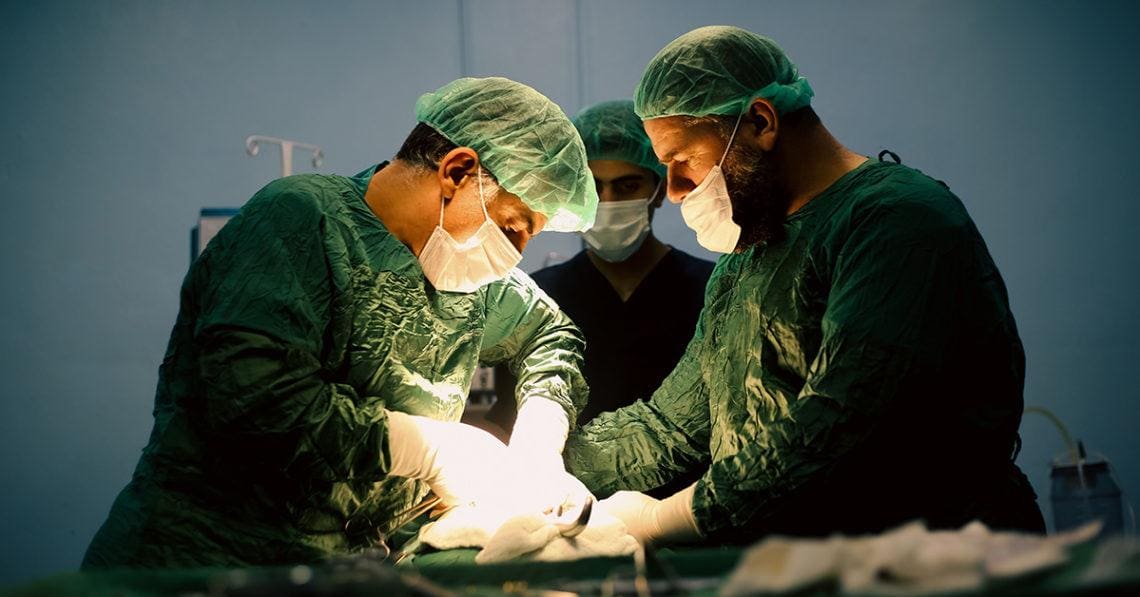
Calls for shedding light on price variability, coupled with an industry that is increasingly consumer-focused, is driving greater examination of how hospitals, payors and providers price and charge for care, and healthcare industry analyst Christina Steiner sets the stage for what to expect in the coming years.
Over the past few years, dual pieces of federal legislation have attempted to curb costs in the healthcare industry, one aimed at hospitals and another targeting insurers. While the initial efficacy of the rules is yet to be determined, they have set a new tone and precedent in the U.S. healthcare industry — namely, that government entities at the federal and state levels are taking a more intentional approach to monitoring and controlling costs that affect consumers.
A Pew Research Center survey found that 61% of Americans believe reducing healthcare spending is a top public priority, only one spot behind the public’s top concern of strengthening the economy. In reducing healthcare spending, there is a recurring theme around price transparency and cost-controlling actions across the healthcare ecosystem. As consumers have called for action, governmental entities, both federal and state, have pushed legislation and regulation to increase transparency around pricing.
Because of the intersection of private and public payors and private healthcare providers and their own proprietary commercial agreements, there has been a veil of secrecy surrounding the cost of healthcare in the United States, clouding a consumer’s ability to make informed healthcare decisions. Greater consumer demand for transparency and government action have paved the way for recent legislation effecting material change in the industry regarding access and affordability, and price transparency.
Recent policies that shaped the current market
The Consolidated Appropriations Act, signed into law in 2020, included the long-discussed No Surprises Act (NSA), which contained key protections to safeguard consumers from surprise medical bills arising from certain out-of-network emergency care and related services. The Transparency in Coverage (TiC) final rule was also released in 2020 by the U.S. Department of Health and Human Services, Department of Labor and Department of Treasury to deliver on the Trump Administration’s initiatives aimed at price transparency in the healthcare sector.
The TiC final rule required most group health plans and health insurance issuers in the group and individual market to disclose price and cost-sharing information to participants, beneficiaries and enrollees. These rules build on HHS actions to increase price transparency by giving patients further access to hospital pricing information through the hospital price transparency rule. That rule requires hospitals to post their standard charges on a publicly available website.
In the two years since their enactment, however, the price transparency regulations have been met with pushback and noncompliance, largely around the lack of adherence to stipulations that require hospitals and certain health plans to disclose prices and negotiated rates.
DOJ’s Civil Cyber Fraud Initiative Could Find Health Care Companies Exposed on Multiple Fronts
The Biden Administration and DOJ intend to pursue cyber fraud through the False Claims Act (FCA), with an emphasis on whistleblower reporting. The implications could devastating for unsuspecting health care compliance teams and lead to multiple exposures to enforcement.
Read moreDetailsFirst in line for compliance: hospitals
The transparency rule, which went into effect in 2021, mandates that hospitals provide clear and accessible price information online, for consumers. The Centers for Medicare and Medicaid Services has provided guidance for hospitals to comply with these requirements, including posting standard charges in two ways:
- A machine-readable file containing a list of all standard charges for all items and services
- A consumer-friendly list of standard charges for a limited set of at least 300 (or as many as the hospital provides) shoppable services.
CMS will deem a hospital as having met the second of these two requirements if the hospital maintains an internet-based price estimator tool. However, this tool must be updated annually, and the hospital must ensure that the tool allows consumers to obtain a personalized, estimated cost, which the hospital anticipates the individual would be obligated to pay. It is worth noting most hospitals choose to utilize this option instead of posting standard charges for shoppable services.
If a hospital chooses to use a price estimator tool in lieu of displaying standard charges in a consumer-friendly manner, the tool must meet the following criteria:
- Provide estimates for as many of the 70 CMS-specified shoppable services that are provided by the hospital, and as many additional hospital-selected shoppable services as is necessary for a combined total of at least 300 shoppable services.
- Allow healthcare consumers to, at the time they use the tool, obtain an estimate of the amount they will be obligated to pay the hospital for the shoppable service.
- Is prominently displayed on the hospital’s website with no barriers to access (e.g., fees, registration).
Since the transparency rule has been in effect, CMS has issued hundreds of written warnings, but did not issue any monetary penalties for non-compliance until nearly two years later. In June 2022, CMS issued its first fines against two affiliated Georgia hospitals, Northside Hospital Atlanta and Cherokee, for noncompliance with the rule. In both cases, CMS issued written warnings and provided each hospital with an opportunity to respond with documentation, but both failed to do so. After four months, CMS reviewed the hospital’s websites and found continued deficiencies and asked both facilities to submit corrective action plans. Both were unresponsive. As a result, CMS imposed civil penalties, fining the institutions $883,180 and $214,320, respectively. Each hospital was accused of the same violations, outlined below:
- Failure for each hospital location to separately make public the standard charges applicable to that location.
- Failure to make public a machine-readable file containing a list of all standard charges for all items and services. Items and services include, but are not limited to, supplies, room and board, use of the facility and other items (generally described as facility fees).
- Failure to publish the required data in a single digital file that is in a machine-readable form.
- Failure to follow the naming convention specified by CMS.
- Failure to make available a consumer-friendly list of standard charges for a limited set of shoppable services.
Although the transparency rule has been in effect for nearly two years, there have been patterns of low levels of compliance, for various reasons, including lack of IT preparedness, financial resources or personnel expertise. However, Turquoise Health recently released its Price Transparency Impact Report, which reflects data from the third quarter of 2022. The company assesses hospital compliance by comparing information found on the price transparency URL for every hospital in the U.S. to CMS requirements. It reported 4,909 hospitals (76%) posted a machine-readable file in Q3 2022 — a significant increase from the previous seven quarters. Though Turquoise Health acknowledged that notable progress has been made, it stated that one in five hospitals received two or three stars, indicating that they either had an incomplete machine-readable file with unhelpful information or a partially complete file with some useful information but was still missing key elements. The organization urged CMS to take a more active stance in penalizing non-compliant systems while recognizing compliant hospitals on its website.
CMS enforces and monitors the rule through a combination of monitoring channels, including periodic audits and review of individual/entity complaints. CMS has governing authority to issue written notices/warning letters, initiate corrective action plans and impose penalties on a scaling factor, driven by hospital size (i.e., bed count) and volume of days in noncompliance. Further, CMS has stated that these monetary penalties will be broken down as follows:
- The maximum daily fine for hospitals with 30 or fewer beds is $300, even if the hospital is in violation of multiple discrete requirements.
- The maximum daily fine for hospitals with at least 31 and up to 550 beds is the number of beds times $10.
- For hospitals with greater than 550 beds, the maximum daily fine is $5,500, even if the hospital is in violation of multiple discrete requirements.
While many hospitals and health systems have been slow to implement the requirements, it remains to be seen whether increases in monetary penalties will impact compliance with the rule. Many hospitals in the nation are currently experiencing significant labor and supply cost increases, which are affecting their operating margins and profitability. Fines and penalties issued by HHS for non-compliance with the transparency rule would further impact smaller-bed facilities or understaffed hospital systems already facing financial and operating challenges.
The second wave of compliance: payors
Following hospitals, payors faced the next wave of federal regulations aimed at fostering a more competitive market for medical treatment. The TiC rules will go into effect in three stages: The first stage originally went into effect Jan. 1, 2022, but enforcement was delayed until July 1, 2022, to allow time for regulated parties to develop and implement machine readable files required for compliance.
The first stage requires health insurers and group health plans to post publicly available, machine-readable files containing rates for all covered items and services between the plan or issuer and in-network providers and allowed amounts for, and billed charges from, out-of-network providers. These files must be available at no cost, without any conditions (e.g., fees, registration), in a standardized form and updated monthly. Additional TiC requirements went into effect Jan. 1, 2023, and others will go into effect Jan. 1, 2024.
Starting this year, payors are required to provide an online price comparison tool (or paper form, upon request) that allows members to receive an estimate of their cost-sharing responsibility for a certain item or service from a specific provider, or providers for 500 items and services, as determined by the departments. The remainder of all items and services will be required in these self-service tools for plan years beginning on or after Jan. 1, 2024.
Many hospital systems have been slow to implement compliance measures in line with the transparency rule; payors, however, seem to be taking an alternate route. Several insurance companies such as UnitedHealthcare, Centene, Anthem and Aetna have already published machine-readable files.
In fact, Turquoise Health reported that 80 insurance carriers published rates — notably, these carriers represent 90% of all commercially insured people. This may be a result of the substantial civil monetary penalties issued by the CMS to hospitals, serving as a cautionary example. CMS also announced the penalties for noncompliance with TiC include requiring corrective actions and/or imposing a civil monetary penalty up to $100 per day (adjusted annually) for each violation and for everyone affected by the violation, a price that will be substantial for larger insurers.
Ultimately, under the regulations, insurers will be required to develop and implement cost pricing tools to enable data-driven decision-making for consumers. Many organizations have already developed in-house tools or outsourced cost estimator tools. More agile startups and organizations with consumer-centric models can facilitate the push to streamlined data consistency and user-friendly interfaces, potentially driving more consistent publication and presentation of data for consumers across the market.
Providers and payors: good-faith efforts at compliance
Although price transparency regulations continue to face resistance in some quarters, CMS has indicated that it intends to enforce the regulations strictly by closely monitoring provider/payor websites and issuing non-compliance letters. Because of inconsistency in methodology and format of hospital machine readable files, CMS has published defined guidelines that serve as compliance roadmaps. Regulated parties should take advantage of these resources and make good-faith efforts toward compliance with the applicable price transparency regulations.
CMS has provided hospitals with various guidance, including:
- 8-Steps to a Machine-Readable File
- 10 Steps to a Consumer-Friendly Display
- Hospital Price Transparency Requirements Quick Reference Checklists
- Corrective Action Plan Response Sample
Payors were also provided with guidance, including:
- Link to GitHub technical specifications for machine readable files
- Link to GitHub validator for the machine-readable files
- 8 Steps to an In-Network Rate and an Out-of-Network Allowed Amount Machine-Readable File
- Technical Clarification Questions and Answers
The federal price transparency regulations have impacted healthcare organizations, portending greater transparency across the industry for costs and shedding light on price dispersion and downstream impacts to patients for out-of-pocket expenses and total costs for care rendered. In addition to increased CMS oversight, the HHS inspector general has become more involved in monitoring compliance with these regulations, specifically with the hospital price transparency rule. The inspector general’s office recently added CMS price transparency oversight to its work plan. The office will audit the CMS monitoring and enforcement controls in place and statistically sample hospitals to determine compliance and whether CMS controls are sufficient to ensure that mandated hospital price transparency information has been made publicly available, as required by federal law.
Given continued monitoring and enforcement activity over these transparency regulations, hospitals and payors should continue to prioritize compliance with the price transparency regulations.



 Christina Steiner is a senior director with Alvarez & Marsal’s healthcare industry group in New York. She specializes in compliance, focusing primarily on operational issues, risk management and process improvements.
Christina Steiner is a senior director with Alvarez & Marsal’s healthcare industry group in New York. She specializes in compliance, focusing primarily on operational issues, risk management and process improvements.